Study Could Explain How Stress Encourages Stomach Ulcers
 “Pavlov demonstrated many years ago that the central nervous system uses environmental signals and past experience to generate anticipatory responses that promote efficient digestion,” said Peter Strick, Ph.D., Brain Institute scientific director and chair of neurobiology at Pitt. “And we have long known that every increase in unemployment and its associated stress is accompanied by an increase in death rates from stomach ulcers.”
“Pavlov demonstrated many years ago that the central nervous system uses environmental signals and past experience to generate anticipatory responses that promote efficient digestion,” said Peter Strick, Ph.D., Brain Institute scientific director and chair of neurobiology at Pitt. “And we have long known that every increase in unemployment and its associated stress is accompanied by an increase in death rates from stomach ulcers.”
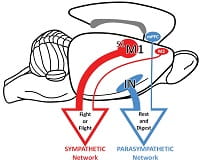 Strick and Levinthal found that the parasympathetic — “rest and digest” — nervous system pathways trace back from the stomach mostly to a brain region known as the rostral insula, which is responsible for visceral sensation and emotion regulation.
Strick and Levinthal found that the parasympathetic — “rest and digest” — nervous system pathways trace back from the stomach mostly to a brain region known as the rostral insula, which is responsible for visceral sensation and emotion regulation.
 These insights also could change clinical gastroenterology practice. Knowing that the brain exerts physical control over the gut gives doctors a new way to approach bowel problems.
These insights also could change clinical gastroenterology practice. Knowing that the brain exerts physical control over the gut gives doctors a new way to approach bowel problems.

